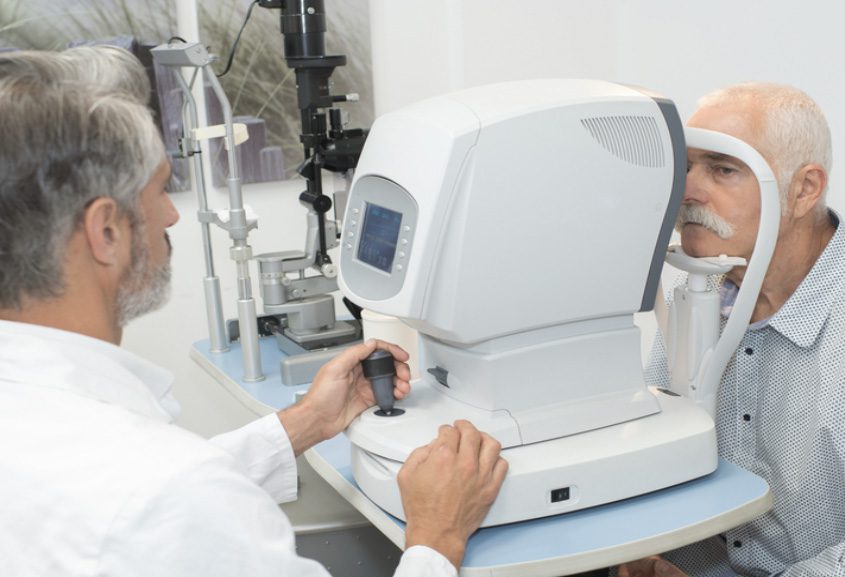
Living Your Best Life With Low Vision
The mission of Living Well With Low Vision is to make it as easy as possible for people to educate themselves about loss of vision and to meet the daily challenges resulting from it. By empowering individuals, we hope to provide practical ways for people to improve the quality of their daily lives and relieve the emotional trauma that often accompanies low vision.
There are four kinds of people in the world:
those who have been caregivers, those who are currently caregivers, those who will be caregivers, and those who will need caregivers.
–Rosalynn Carter